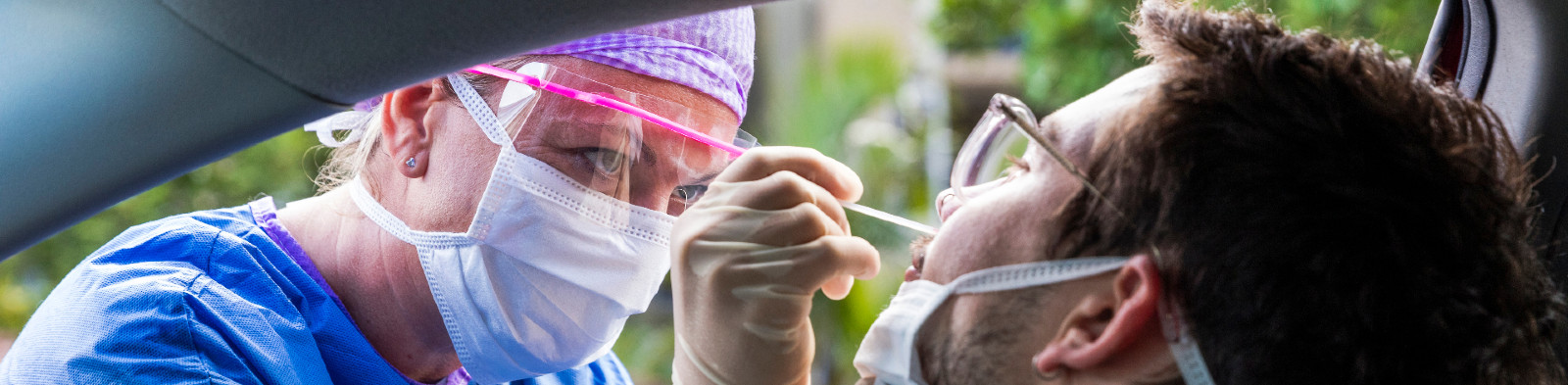
How the pooling of samples could help increase testing capacity for COVID-19
Research shows that when a reliable estimate of infection rates is unavailable, adaptive sized pool testing could offer increased efficiency when screening for infections such as COVID-19.
The emergence and spread of coronavirus disease 2019 (COVID-19) has placed enormous stress on health systems worldwide. Widespread testing is often seen as a crucial response to such a pandemic. Through testing, those infected can be identified and consquently they and their contacts can begin the period of isolation which can help prevent further spread. Testing also informs policy planning by identifying infection clusters in the population. Such measures can help reduce the strain on health services, which has been a priority for governments around the world.
However, the equipment, material, and labour required for testing is limited, thanks in part to a surge in global demand, making it a challenge for even high-income countries to conduct on a large scale.
Pooling of samples has the potential to reduce the number of tests required for screening a population with a low infection prevalence. The process is not a new one, and has been successfully used to expand testing capacity for other infectious diseases. It involves the testing of pools of fixed-sized samples instead of individual samples. A negative outcome within the pool implies a negative outcome for all samples in the pool, and no further tests are required. When a postive result is found though, all constituent samples of that pool are tested. Since negative pools do not need further testing, this approach has the potential to substantially reduce the number of tests required.
New research from Dr Navid Izady at Cass Business School provides a detailed analysis of this strategy. It finds that it could substantially reduce the number of tests required as compared to individual testing. However, fixed-size pooling's efficacy depends on there being a reliable estimate for prevalence of the virus in the target population. Errors in the estimation of prevalence could signficantly reduce the benefits of pooling, or even in extreme cases make it more expensive than individual testing.
If a reliable estimate of infection rate is not available, taking a limited random set of samples from the population and testing them individually, combined with expert judgement, would provide a probability distribution of prevalence. If the resulting distribution is not highly variable, a two-stage pooling strategy with a fixed pool size can still be applied.
However, if the initial distribution is highly variable, the research recommends the use of a multi-stage adaptive pooling strategy. Here, the optimal size of the pool in each stage is based on the most up to date distribution of prevalence, combining the information from initial distribution and the test outcomes in previous stages. The distribution is updated dynamically as more tests are conducted.
Adaptive pooling could prove more time-consuming than two-stage pooling, as pools need to be tested sequentially. To address this, the population of samples can be divided into a number of sub-populations depending on the parallel processing capacity of the lab. These sub-populations can then be tested in parallel using the adaptive approach, utilising the lab's full capacity and providing the results in a shorter time.
Analysis shows that when the variability of prevalence is high, a multi-stage adaptive approach could reduce the expected number of tests as compared to two-stage pooling by as much as 12%. At a time when government funds are under immense strain, such efficiencies could prove extremely valuable.
The pre-published version of the research paper Pooling of Samples to Increase Testing Capacity for COVID-19 can also be downloaded at the link below.